With warm weather, we always see an increase in the number of parvovirus cases at Animal Emergency Clinic. So I decided to put together some information on a virus that is common in the United States, with our local High Desert being no exception. I hope to shed light and clear up some of the myths and misinformation about parvovirus.
What is Parvo?
Canine parvovirus (or CPV) is a virus that was discovered in the 1960s and named CPV-1. This initial strain caused only mild diarrhea in dogs. The next strain, CPV-2 was discovered in 1978 and was more severe, with myocarditis and congestive heart failure as potential secondary effects. Since then, several new strains have popped up over the years. At the moment, CPV-2b is the most common strain throughout the world. (Mazzaferro, 2013)
Symptoms
| Acute vomiting | *Diarrhea – often bloody | Abdominal pain |
|---|---|---|
| Malaise | Pyrexia | Anorexia |
The hematochezia (bloody stool) is caused by the destruction of intestinal crypts.
Who gets it?
- Puppies or unvaccinated dogs generally between 6-20 weeks of age, but older
unvaccinated dogs can contract it as well. - Studies show Dobermans, Rottweilers, Pitbulls, and German Shepherds are the
most susceptible (Mazzaferro, 2013). - Gender does not seem to play a role in virus selection, except in dogs over 6
months of age. For unknown reasons, unvaccinated intact male dogs over 6
months of age are more likely to contract it. (Mazzaferro 2013)
How is it transmitted?
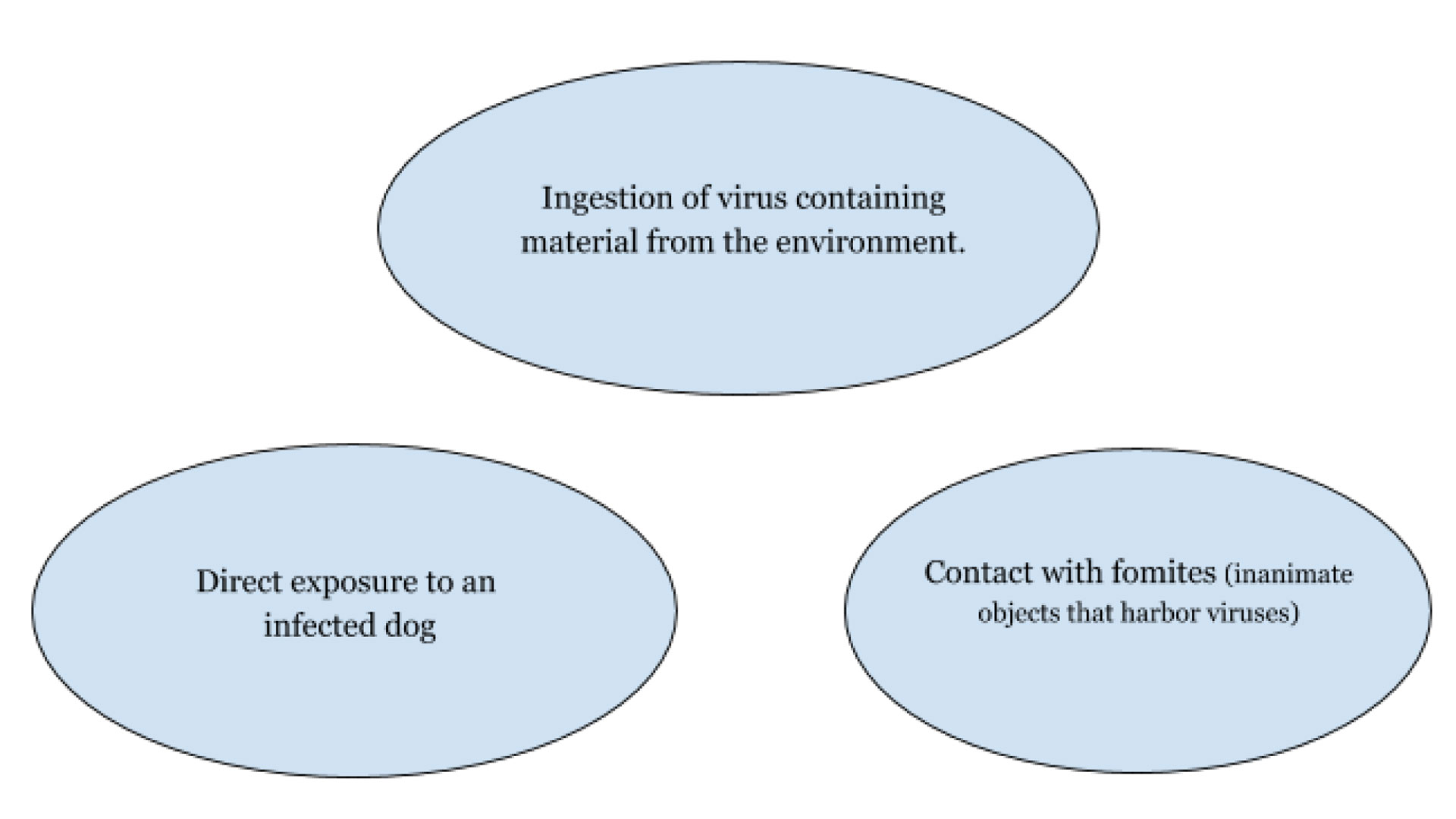
Parvovirus is not an airborne virus, but it is highly contagious. It can easily be passed from dog to dog or through exposure to fomites with virus-containing material. It starts in the oropharyngeal lymphoid tissue, enters the bloodstream and the intestinal crypt epithelium is infected by day four. Clinical signs are seen 4-10 days after infection. (Li, 2015)
How is it diagnosed?

There are many types of tests available to test for parvo. Currently, the most widely used is the ELISA snap test (enzyme-linked immunosorbent assay) because they render a result within 10 minutes. They have a sensitivity between 56-81%, so patients with a negative result whom we are still suspicious of parvovirus, should be retested in 36-48 hours. (Li, 2015)
Reasons for infection
1. Failure of passive transfer of antibodies.
Generally, mom was not vaccinated or the puppies did not receive colostrum. Colostrum from a vaccinated mother is critical for initial protection for the pups. (Bassert, 2017)
2. Lack of vaccination, or improper vaccination
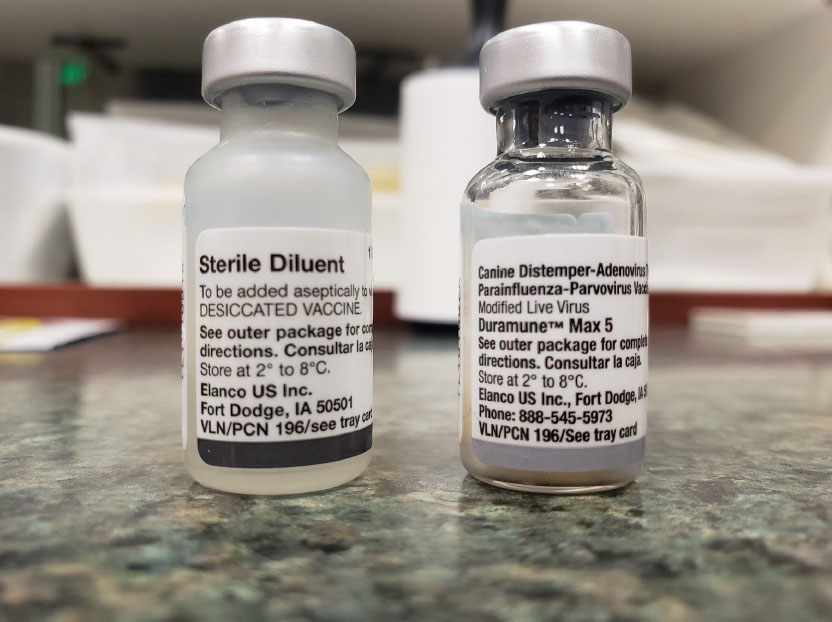
There are two parts to an infectious vaccine, a lyophilized (freeze-dried) portion, and a diluent that is formulated with the correct pH and preservatives. The lyophilized portion is reconstituted with the diluent, and only stable for one hour. If the vaccine isn’t stored, handled, or administered properly, it’s effectiveness comes into question. (Bassert 2017)
Another reason is if the vaccine is not administered at the correct intervals or at all. A series of vaccines is recommended generally starting around 6-8 weeks of age and continues every 2-3 weeks until the puppy reaches 16 weeks of age.
3. Maternal immunity preventing a vaccine response
This is least likely, and rare, but possible. The length of time the mother passes antibodies onto the pups varies and can interfere with initial vaccination. However, in rare cases like these, if a puppy is vaccinated correctly, at a veterinarian, with proper documentation, the vaccine company will generally reimburse the owner for the cost of treatment.
Prevention
When you get a new puppy, follow up with your veterinarian immediately to get them started on a vaccine schedule. Besides that veterinarians have the training and knowledge on vaccine schedules, storage, handling and administration of vaccines, the vaccine company will not “back up” their product unless it was administered by a veterinarian correctly.
Isolate your puppy until they’ve received all of their initial vaccines. Trips to the park, walks, and trips to the pet store should be avoided until they have completed their vaccine series. They are not fully protected until they have been fully vaccinated.
When you take your puppy for vaccinations at your veterinarian, you should ideally carry them and not let them congregate with other dogs in the lobby.
As for fomites: imagine a doorknob that a person with the flu touches right before you. The same goes for dogs. We can do everything we can to isolate our puppies until they are old enough to go out into the world, but you can bring it home on your shoes unknowingly.
What should I do if I suspect my dog has Parvovirus?
Take them to a veterinarian as soon as possible. Any puppy with vomiting or diarrhea should be evaluated as soon as possible. In a parvo patient, the longer you wait to seek treatment, the harder it will be to prevent death. It will also likely be more costly for you, as they will most likely require more extensive care to get them back. Many owners find themselves in a bind, unable to pay for examinations or parvo tests, let alone parvo treatment. It’s a situation where hindsight is 20/20, but the best solution I can offer is to try to be financially prepared when you take on a
pet. It’s critical to have the funds for basic care such as vaccinations and it’s a good idea to have a backup plan, such as an emergency fund or line of credit available to you in case of emergency.
Laboratory Findings
Many times, veterinarians are asked why blood work and repeat blood work is necessary, especially when the cost is a concern. The vomiting, diarrhea and anorexia a parvo positive patient experiences, often cause decreased levels of electrolytes, proteins, and glucose and elevation of their kidney enzymes. Excessive vomiting and diarrhea can also cause a state of hypovolemic shock. This essentially means that not only are they dehydrated, but that they have lost much of the plasma or “fluid” portion of their blood due to dehydration. Lab tests such as blood gas analysis tell us information about their perfusion, oxygenation, and ventilation and electrolyte status. Chemistry panels tell us information about their organ function. Complete blood cell counts (CBCs) evaluate their red and white blood cell counts and function. Parvo patients often have a low white blood cell count in response to the virus. All of this information collected is very valuable in guiding treatment. Supplementation of intravenous electrolytes and glucose can be adjusted based on lab work, protein can be restored with transfusions, enteral, or parenteral nutrition.
Mortality Rate
Parvovirus has a mortality rate of 91% without treatment, and depending on the circumstances, as low as 4% with treatment (Perley et al., 2020). That means the disease will most likely be fatal in untreated patients. It all depends on the severity and the interventions taken. Even with gold standard treatment, some patients will not make it, but they have a much higher chance of survival.
Treatment
There are often two main options that will be offered to you if your puppy is diagnosed with parvovirus, inpatient and outpatient.

Sinuhe Flores, Practice Manager at AEC working on a parvovirus patient
Inpatient treatment has a much better chance of success in my clinical experience. It can be as basic as intravenous fluids, anti-vomiting medication, pain medication (parvo is painful!) antibiotics, and anti-diarrheal medication and it may be as extensive as nasogastric feeding tubes, parenteral nutrition, blood product transfusions, additional medications, etc. It all depends on the puppy’s current status at the time of hospital admission, the severity of the virus, and how the individual animal responds to treatment.
Outpatient treatment can also be successful and are solely chosen due to cost concerns. It’s usually only recommended in mild cases, or cases that are caught early. It may involve daily anti-nausea and antibiotic injections, and subcutaneous fluid administration. Subcutaneous fluids are given under the skin instead of intravenously. They work by being absorbed by the capillaries and eventually into the bloodstream. Oral medications are not generally recommended, as the patient very well may vomit them up before they can take effect, or not be absorbed properly due to the patient’s altered physical state.
Colorado State University did an interesting study on outpatient Parvo protocols in 2013 (Venn, Preisner, Boscan, Twedt, & Sullivan, 2016), and the University of Pennsylvania followed up with another outpatient Parvo study in 2018 (Perley et al., 2020). Both of them had a success rate in the 80% range. However, for both programs, outpatient treatments were started on intravenous fluids first if they were in a state of hypovolemia. They also regularly monitored their electrolytes and other basic lab tests, along with injectable medications. Therefore, they were much more aggressive, and therefore more effective than your average outpatient choices.
Obstacles & Complications
Some obstacles are almost certain to occur. Parvovirus patients may suffer from hypovolemia, hypoperfusion, hypoglycemia, anemia, acid-base disturbances, pain, arrhythmias, sepsis, intussusception, and even death despite our best efforts. Aggressive in-hospital treatment, as early as possible, is our best bet in avoiding negative outcomes. Many times, I’ve seen owners rush in on day four or five of their puppy being sick, and it can be very difficult to bring them back.
Disinfection
If you have a Parvovirus positive dog, be aware that they can shed the virus for 39 days post-infection, and should be isolated from other dogs. Use dilute bleach to disinfect any surfaces you can (1 part bleach to 32 parts water) (Mazzaferro, 2013). You should not bring any unvaccinated dogs into your home for at least a year, as furnishings cannot be thoroughly disinfected. Dispose of feces promptly and do not allow other pets to be exposed to it.
Conclusion
Parvovirus can often be easily prevented through proper vaccination and isolation. It can also be treated with both inpatient and outpatient protocols. Inpatient protocols are superior, but not the only option, especially if you bring them in quickly after they begin exhibiting symptoms.
References
Bassert, J. M., VMD. (042017). McCurnin’s Clinical Textbook for Veterinary Technicians, 9th Edition [VitalSource Bookshelf version]. Retrieved from vbk://9780323394611
Li, R., & Humm, K. (2015). Chapter 97 Canine Parvovirus Infection. In Small animal critical care medicine (2nd ed., pp. 509-513). St. Louis, MO: Elsevier.
Mazzaferro, E. (2013). The Parvo Puppy: What is the best approach and what’s new? International Veterinary Emergency & Critical Care Symposium. Retrieved June 18, 2020
Perley, K., Burns, C. C., Maguire, C., Shen, V., Joffe, E., Stefanovski, D., . . . Watson, B. (2020). Retrospective evaluation of outpatient canine parvovirus treatment in a shelter-based low-cost urban clinic. Journal of Veterinary Emergency and Critical Care, 30(2), 202-208. doi:10.1111/vec.12941
Venn, E. C., Preisner, K., Boscan, P. L., Twedt, D. C., & Sullivan, L. A. (2016). Evaluation of an outpatient protocol in the treatment of canine parvoviral enteritis. Journal of Veterinary Emergency and Critical Care, 27(1), 52-65. doi:10.1111/vec.12561

Laura Waller is an RVT at Animal Emergency Clinic in Victorville, Ca. She is married and her and her husband share their home with a menagerie of dogs and cats. She is currently working on her BASc in Veterinary Technology and aspires to become a VTS in ECC.





Leave A Comment